|
Melody Wu Fifteen minutes. That’s the average amount of time physicians in the United States spend with each patient. Those days, weeks, and even months spent in pain all reduced to a brief, fifteen minute visit. One medication, one quick reassurance, and you are sent on your merry way home. Except, you aren’t really merry. This is the issue with the US healthcare system.
You see, Western medicine uses a reductionist approach. Physicians are trained to analyze parts of the body, parts of a disease, parts of a virus, and so on. Every disease is broken down into separate symptoms to analyze, and medications are prescribed to treat each one individually. As a result of this, Western medicine consists of a lot of short term, effective solutions that create immediate responses. We’ve all experienced its benefits before. Popping a Tylenol to quickly ease a pounding headache. Swallowing a few allergy pills to alleviate the unbearable sinus congestion and aggravating itchiness. Quick and easy. These accelerated results prove Western methods to be highly effective for treating severe illnesses, as time is vital in emergency situations. Here is the issue, though. What happens after? Western medicine fails to address long term plans for patients to return to optimal health and prevent future occurrences. Even if it is mentioned, it is often brushed upon quickly with no follow up. For example, a patient comes in with insomnia. A Western doctor would listen to the symptoms, make a differential diagnosis, and prescribe the appropriate medications. The issue is this: the pills don’t resolve the underlying cause of the insomnia. The overanxious mindset, the external stressors of work and family, the lack of proper nutrition, whatever it may be. Those are the harder things to manage, but they are the most important. This lack of prevention leads to a large number of patients suffering unnecessarily from chronic diseases, without the tools to properly combat the root causes of their issues. According to the CDC, 70% of deaths are due to chronic illness. The cost of chronic care per year is $1.5 trillion, or 75% of all medical expenses; and yet only a small fraction of the medical budget is spent on preventative care. Though there is overwhelming evidence that prevention is key to minimizing costs and maximizing health, Western medicine still fails to prioritize it. The length of each physician visit is only getting shorter and shorter, as doctors struggle to bring in enough patients to cover the rising expenses of running a hospital or clinic. This is where Eastern medicine comes in. Eastern medicine employs a holistic perspective. It focuses on the person as a whole, and views health as a delicate balance between the body, mind, spirit and environment. Rather than targeting solely the initial complaint, the physician prioritizes equipping the patient with the proper tools and knowledge to better adapt to their environment. It is about strengthening the internal defense mechanisms to prevent the disease from even occurring in the first place. This all takes place through implementing healthy habits, being mindful and accountable, as well as consistent follow-up with patients. Visits with doctors are often an hour or longer, where the doctor really takes the time to get to know the patient as a whole. The physician takes into account all the different social determinants of health--understanding the patient’s family, job, economic situation, stressors, hobbies, etc. As opposed to the passive role in Western medicine, patients take up an active role in creating their own personalized treatment plan. Eastern medicine recognizes that everybody’s body does not respond to the same treatments in the same way. We’re all different, and we must take those differences into account. This all sounds pretty great, right? Why doesn’t everyone do this? We live in a society where immediate results are favored. Though Eastern medicine promises longevity and improved happiness, it takes a long time to see results. It requires discipline to maintain these habits -- eating healthy, exercising often, changing your mindset. In addition to this, creating these longer sessions requires a complete upheaval of the current US healthcare system. The sad reality is that the supply simply cannot meet the huge demand. It’s hard to change. But there are steps being made in the right direction through institutions like the UCLA Center for East-West Medicine, among other integrative organizations. For us, the ordinary people, a great first step is to recognize the intricate interplay between our body, our mind and our environment. Be mindful about the factors in your life that affect your health. What stresses me out? What foods feel right for my body? What type of exercise is best suited for me? Through this awareness, we can begin to form our own individualized plans to optimize our health and happiness.
0 Comments
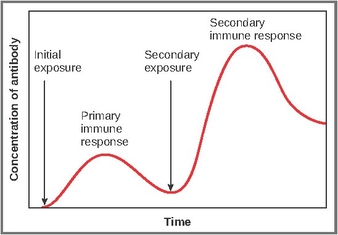
Caitlyn Tran 5.4 is greater than 0 and 0 is less than 5.4. With the basic rules of math, comparing these numbers seems so simple, yet they become more complex when applied to topics like representation. As of 2016, Asian Americans and Pacific Islanders (AAPIs) make up approximately 5.4% of the United States population. Although that does not sound like much, this mere 5.4% translates to over 16 million people. With such large variations between different ethnic groups, including but not limited to differences in socioeconomic levels and differences in culture, it makes sense that their health and medical needs may differ too and that representation in clinical trials is needed. However, this has not been the case, as seen with how the racial and ethnic minorities that make up approximately 30% of the United States population only constituted 18% of clinical trial subjects in cancer clinical trials funded by the National Cancer Institute between January 1, 2003, and June 30, 2005. This indicates that some barriers must be responsible for the discrepancy between clinical trial representation and minority representation in the United States population. Multiple studies have confirmed this by providing insight into what those barriers may be. Myths about AAPIs being a healthy minority, problems with informed consent, and mistrust in healthcare are a few that have been brought up. Clinical trial representation could potentially increase if the aforementioned barriers are addressed. For instance, healthcare professionals could play a larger role in increasing trust in healthcare by being more culturally aware and sensitive in addition to making a larger effort to recruit more AAPI members to participate in clinical trials. This topic has become even more significant in light of the distribution of two COVID-19 vaccines: one by Pfizer/BioNTech and the other by Moderna. In the past, there have been several different vaccine types, which contained different components: inactivated or weakened virus, harmless fragments of proteins or protein shells, a viral vector in which a virus is genetically engineered to generate proteins, or RNA or DNA genetically engineered to generate proteins. Regardless of the type, each vaccine has been designed to elicit a primary immune response. This way, the body can manufacture memory cells and other immune cells required to elicit a faster and more effective secondary immune response if the body ever comes across the actual pathogen. Since the COVID-19 pandemic began, the pressure to quickly produce a vaccine has encouraged scientists to explore a new type of vaccine: an mRNA vaccine, which was used by both Pfizer/BioNTech and Moderna. Once the COVID-19 vaccine is administered to muscle in the arm, muscle cells can use the mRNA to produce spike proteins found on the surface of the actual SARS-CoV-2 virus before breaking down the mRNA. The proteins still generate an immune response, but the mRNA cannot cause the virus nor does it interfere with a person’s genetic material. This makes the vaccine safe and open for everyone to take unless they have had an allergic reaction to any past vaccines or COVID-19 vaccine components. However, further details should be discussed with primary care doctors or relevant healthcare specialists. Even with these details about how the vaccine should theoretically work, the safety and efficacy of a vaccine ultimately boils down to clinical trial results, which brings us back to the matter of representation in clinical trials. As supported by evidence that clinical trials are becoming more diverse, the vaccine by Pfizer/BioNTech clinical trial racial and ethnic distribution included 26.2% Hispanics/Latinos, 9.8% African Americans, 4.4% Asians, and less than 3% other minorities. Similarly, Moderna’s vaccine clinical trials included 20% Hispanics, 9.7% African Americans, 4.7% Asians, and less than 3% all others. With so many different racial and ethnic groups present in the United States population, these clinical trials could be more diverse. However, the breakdown of the recent COVID-19 vaccines indicates that we are taking a step in the right direction. Hopefully, this trend continues and AAPI along with other minority representation in clinical trials will improve both health results and trust in healthcare. Since AAPIs represent about 5.4% of the United States population, they should also be represented in clinical trials. After all, 5.4 is greater than zero. Sources:
Calvin NguyenThe coronavirus is a naughty little thing that has caused people to raise their eyebrows.
It's a bit worse than that. The coronavirus is the actual spawn of the devil and will cause Rapture to begin early. Not as bad as that. The coronavirus is a serious threat that we as a community should take seriously. Yes, it is in Los Angeles. Yes, it is dangerous for elders and those with underlying conditions. But no, it is not a Chinese bioweapon that is going to kill half of the planet. To keep ourselves and the community healthy, we have to be vigilant and do our best to promote a healthy environment. To prevent yourself and others from getting sick, make sure to follow a few guidelines: Wash your hands. You should be washing your hands regardless of a global pandemic, but make sure to wash your hands with vigorous passion now; on a molecular level, the coronavirus is surrounded by oily material, and soap does wonders in dissolving and removing these substances from your hand. Many only spend five seconds at the sink, but embrace the gentle sensation of flowing water for at least twenty seconds. Sing “Twinkle, Twinkle, Little Star”. Sing the chorus of Aqua’s “Barbie Girl” twice. I’m not afraid to say that I prefer the latter. Don’t touch your face. If your hands happen to be dirty, then touching your mouth, nose, or eyes could provide invasive microbes an easy entry point into your body. Don’t give them that chance- make the coronavirus’ debatably non-existent life as difficult as possible. Be sanitary. There are only two situations where sharing is not caring. Communism, and Infectious Outbreaks. If you’re sneezing or coughing, do it in the proper direction, like your elbow. Refrain from coughing into people’s faces. You might get them sick, and it’s not very nice to do so in the first place. It may be a good idea to wear a facemask. Although facemasks aren’t very effective at keeping you safe from viruses, they ARE effective at quarantining your germs to yourself. These masks begin to lose their effectiveness once damp, so be sure to change it when needed. If you feel that a face mask isn’t enough, a gas mask and hazmat suit would probably eliminate any possibility of contracting the virus (this does have the unfortunate side effect of instilling terror in your peers, but depending on who you are, this can be a positive). SEEK MEDICAL ATTENTION EARLY. The coronavirus has many symptoms, such as coughing, fever, exhaustion, nausea, runny or congested noses, and sore throats. If you believe you are developing these symptoms, please consult your physician. Yes, these symptoms do sound like any normal flu, but that’s all the more reason why we need to be monitoring our health. Better safe than sorry, especially when the “sorry” entails a school shutdown. Think about the safety of your friends and classmates. Nobody wants to be known as the person who accidentally infected the entirety of their club. This is the time to be responsible. One more thing- just because someone looks Asian and has a cough does not mean he or she is the secret harbinger of global armageddon. Quite frankly, as a Vietnamese-American who has never stepped foot in China, and much less Wuhan, I’m a bit tired of my Lyft driver acting like I have Ebola just because I can’t seem to get rid of my cough after a month. No, John, I’m not Chinese. Yes, John, I’m fairly certain I’m not about to infect the entirety of UCLA. Please just drive me to my Care Extenders shift. Thank you. Five stars. Be smart. Stay healthy everyone. |
Archives
April 2021
Categories |